Feature / Wearable wins
 Time and again it is said that patients and NHS services benefited from the rapid adoption of digital technology during the Covid pandemic. Video links allowed patients to consult with their GP without either party risking catching the virus. Wearable sensors, measuring vital signs such as blood oxygen levels, heartbeat and blood pressure, helped move patients out of hospital, freeing up beds and reducing infection risk.
Time and again it is said that patients and NHS services benefited from the rapid adoption of digital technology during the Covid pandemic. Video links allowed patients to consult with their GP without either party risking catching the virus. Wearable sensors, measuring vital signs such as blood oxygen levels, heartbeat and blood pressure, helped move patients out of hospital, freeing up beds and reducing infection risk.
These experiences pointed to a future in which inpatient beds are reserved for the sickest, while those with chronic disease live in their own homes or care homes when not in the acute phase of their illnesses.
Most consumers interested in health will be aware of the rapid development of digital watches that can track heartbeat, distances run or walked, even blood oxygenation. While most of these are not medical grade devices, there have been advances in clinical medical technology, or med tech, with new and smaller wearables freeing up patients to move around without being tethered to bedside monitors.
In this new world, the NHS must be fleet of foot, adopting the technology required to support patient and staff needs. Finance staff will play an important role – supported by the HFMA’s Delivering value with digital technologies programme.
The programme, which is supported by Health Education England, aims to increase awareness of digital healthcare technologies among NHS finance staff, while enabling finance to take an active role in supporting the use of digital technology to transform services and to drive value and efficiency.
The adoption of new technologies is not straightforward. There is opposition from patients who may not have access to the internet, or are less comfortable with technology.
Some sections of the media want clinicians, particularly GPs, to offer more in-person consultations, rather than by video link. And, with insufficient evidence collected, there are questions over whether digital is a more efficient use of resources.
Work remains to be done to ensure the changes have an impact on underlying issues identified before the pandemic, says Nuffield Trust fellow Rachel Hutchings (pictured). She has researched digital adoption in the NHS, including a report last year on practical steps for implementing digital innovations.
 Training of clinical and non-clinical staff is vital, she says. ‘We found in our work that when implementing digital technology, it’s not just a case of putting it in and expecting it to work. Training is really important. And there are underlying issues, such as variation in the adoption of digital technologies across health and social care. There are still deficiencies in digital maturity in NHS organisations.’
Training of clinical and non-clinical staff is vital, she says. ‘We found in our work that when implementing digital technology, it’s not just a case of putting it in and expecting it to work. Training is really important. And there are underlying issues, such as variation in the adoption of digital technologies across health and social care. There are still deficiencies in digital maturity in NHS organisations.’
She adds that integrated care systems will be taking a greater role in managing and developing digital across their areas, providing an opportunity to address digital needs.
‘We can see there’s huge potential and opportunities in med tech for improving the experiences of patients and staff, and in the running of the wider healthcare system. For example, during the pandemic, patients saw a lot of the potential for increased access through remote monitoring, improved options for self-management of long-term conditions, or through providing an alternative for greater choice.’
Ms Hutchings adds that there were also benefits in social care, with staff and clients seeing the potential to use data more effectively and provide more joined-up care.
In-person options
Despite the enthusiasm in the health service for the possible gains to be made, she insists face-to-face consultations must remain open for those who don’t want to – or cannot – access digitally based services.
In developing digital tech, the health service must take care to be guided by real needs, rather than just opting for the latest gadgets. ‘We identified in our work that there had to be support to implement different types of medical tech. There must be co-design, working with users, patients and staff to understand what they need and make sure the technology is appropriate for the population,’ Ms Hutchings says.
As well as matching an organisation’s digital maturity, new tech must match local people, she argues. There is no point in replacing face-to-face appointments with a digital monitor if the cohort of patients are not willing to use it or are unlikely to feel reassured by it.
Nevertheless, many in the NHS and the government, as well as NHS England and NHS Improvement, believe the rapid adoption of technology during the pandemic has shown the way for the next stage of the service’s development.
A lot of excitement surrounds the use of technology to facilitate virtual wards. These are ‘wards’ of patients often with similar disease types living at home. Their health can be monitored using wearable devices, which can report directly to the provider’s clinicians or with the patient inputting their data via a tablet. This is supplemented by video and phone calls.
While virtual wards can be facilitated by technology, they do not always need a digital element, Ms Hutchings insists. ‘For most people with long-term conditions, it’s about how technology can support them and enable greater access. It’s not necessarily a replacement, but to complement and enable healthcare. Technology is not an end in itself.’
NHS England and NHS Improvement have requested that integrated care systems (ICSs) work with providers to develop and expand the use of virtual wards over the next two years. ICSs have been asked to ensure that there are 40 to 50 virtual wards per 100,000 population by December 2023.
The national bodies have provided £200m in 2022/23 to support this, with £250m on a match-fund basis in 2023/24. ICSs will be expected to fully fund their virtual wards from 2024/25.
Norwich virtual ward
Norfolk and Norwich University Hospitals NHS Foundation Trust has established a 24/7 virtual ward to support patients who would ordinarily require an acute inpatient bed to continue their recovery in their own home, or monitor their condition in the run-up to an operation.
The virtual ward has the capacity for up to 40 patients who can be transferred from inpatient wards, direct from clinic and from the emergency department. Virtual ward rounds and phone or video calls via a provided tablet are made daily. Patients wear a sensor that monitors skin temperature, pulse, and oxygen saturation levels remotely, with the information recorded in the clinical dashboard. Blood pressure can also be taken when required.
Patients can contact clinicians directly by pushing a button on the screen should they have any concerns between the ward rounds. The virtual ward patient kit includes a modem to provide internet access, overcoming concerns that virtual ward programmes could exclude some patients without an internet connection.
Patient feedback has been overwhelmingly positive about the service, which has seen more than 1,100 patients to date since implementation in February 2021, releasing more than 7,700 inpatient bed days.
Emily Wells, chief nursing information officer, says: ‘We’re making great strides in modernising our services across Norfolk and Waveney and embracing digital services with the advantages they bring to patients and colleagues. Even though we started behind other health systems in terms of digital maturity, our virtual ward is performing exceptionally well with fantastic patient feedback.’
Virtual ward manager Claire Beard adds: ‘The feedback has been overwhelmingly positive. Patients being able to be in their own bed makes such a huge difference and aids their recoveries.’
Patients with irregular heartbeats normally spend two or more days in hospital being closely monitored to assess how they react to treatment. But thanks to a new virtual ward, up to 120 University Hospitals of Leicester NHS Trust patients with atrial fibrillation (AF) can remain at home during the close monitoring phase. AF, which affects 1%-2% of the general population and 10% of those over 70, is associated with an increased risk of stroke compared with those with a normal heartbeat.
In a pilot, patients were given equipment to monitor their blood pressure, heart rate and oxygen levels, and a device to produce an electrocardiogram (ECG), which assesses heart rhythm. An app sends the data to virtual ward clinicians.
The full service has now been launched with £274,000 of funding from the NHS England transformation directorate (formerly NHSX) in association with tech specialist Dignio.
Future of care
Andre Ng, consultant cardiologist and electrophysiologist at the trust, says: ‘This is a glimpse into the future of care for patients with atrial fibrillation. This service allows patients to be managed and recuperate in their own homes whilst their heart rhythm settles back to normal, but with the peace of mind that they’re still being monitored by specialists.
‘We have already received great feedback from the patients treated, and have successfully managed patients with reduced hospital stay and avoided admission or readmissions.’
Liverpool Heart and Chest Hospital NHS Foundation Trust (LHCH) is using similar remote monitoring to help patients with arrhythmia, including AF, stay at home during the initial observation phase. Patients wear a compact showerproof device for up to 14 days, which collects data on the heart rhythm. The device is then posted to LHCH’s partner, iRhythm, for fast analysis using artificial intelligence.
’We believe this has significantly improved patient outcomes across the trust, as patients with undiagnosed and unmanaged heart rhythm conditions are much more likely to have recurrent symptoms such as blackouts or palpitations and some may even progress to a stroke,’ says consultant cardiologist Jay Wright. ‘We see this service as a fantastic new tool in our efforts to prevent this.’
Waiting times for ECGs fell from six weeks to a matter of days during a pilot of the technology. By avoiding the pinch points in the traditional methods of diagnosis, which may involve overnight stays in hospital and repeat testing, the scheme has freed up beds and other resources.
The trusts implementing medical technology emphasise the benefits to patients, yet there are also potential savings, such as reduced bed days and the avoidance of costly, often invasive, diagnostic procedures.
Nuffield Trust’s Ms Hutchings says efficiency should be a byproduct of schemes that use technology to improve care to patients, repeating that the technology should not be an end in itself. ‘You’ve got to be careful if you are seeing tech as a way of cost saving. It has to support your plans and not just save money. Technology also requires ongoing investment to make it sustainable – it is not a quick fix,’ she says.
‘How do you enable the right patient to be treated in the right place at the right time? How do you support people when they don’t need to be in hospital? There’s potential for cost savings, but the primary aim must be to treat patients appropriately.’
Digital medical technology has great potential in the NHS and the service is already using it to move or keep patients out of hospital, open up pathways or provide new treatment. However, the focus of the service must be on making changes that benefit patients and staff.
• Click here for more on delivering value with digital technologies. The programme has also published case studies on remote monitoring here.
Clot preventer
 A venous thromboembolism (VTE) or blood clot is a common and potentially fatal complication of acute stroke, occurring when patients have less mobility due to prolonged recovery or bed rest after a stroke. Blood flow to the legs is reduced, making clotting more likely.
A venous thromboembolism (VTE) or blood clot is a common and potentially fatal complication of acute stroke, occurring when patients have less mobility due to prolonged recovery or bed rest after a stroke. Blood flow to the legs is reduced, making clotting more likely.
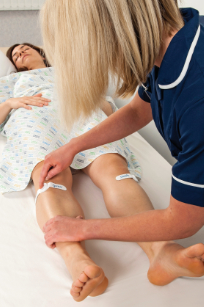
However, a small wearable device, being used at the Royal Stoke University Hospital and others, is helping prevent VTE by increasing blood flow to the lower limbs and back to the heart.
The Geko device is being used as an alternative to more standard VTE prevention. The existing treatment – known as intermittent pneumatic compression (IPC) – uses a small plastic sleeve worn around the leg that is inflated periodically to squeeze the calf, which increases blood flow.
Indira Natarajan, consultant stroke physician and clinical director of neurosciences at the University Hospitals of North Midlands NHS Trust, says IPC is an effective method of VTE prevention. But 30% of patients are contraindicated or unable to tolerate IPC due to medical conditions, such as fragile skin, or noise from the electric pump disrupting sleep. There was no alternative to IPC to prevent blood clots in these patients, he says.
The National Institute for Health and Care Excellence has supported the use of Geko for these patients. Professor Natarajan says the Geko device is small – about the size of a wristwatch – and worn at the knee. ‘It gently stimulates the common peroneal nerve, resulting in increased blood flow in the deep veins of the calf, equal to 60% of walking, without a patient having to move. It is comfortable for patients to wear and simple for staff to administer.’
It could be used across the NHS to address post-stroke VTE prevention, he says. ‘Real-world data from a review of 2,000 acute stroke patients at the Royal Stoke University Hospital reported the device is safe and well tolerated and led to a 46% reduction in VTE,’ he adds.
‘Nursing staff prefer Geko as it does not have to be connected and disconnected when patients get out of bed. It’s also less likely to be soiled by incontinent patients.’
While Geko and IPC have similar costs, the former has been shown to deliver a cost saving to the healthcare system, he says. ‘Six days’ use of Geko in acute stroke is estimated to save the NHS £337 per patient, when no other VTE prevention can be prescribed.’
Related content
HFMA London Branch, SDN and London Finance Academy look forward to welcoming you to the Annual conference 2024
This event will bring together professionals from the finance and technology sectors to explore the power of AI within NHS finance.